Volume 6, Issue 3
March 2026
Motivators and Barriers to Choosing Ophthalmology Among Saudi Medical Students: A Cross-Sectional Study
Abdulmajeed Al Khathami, Nada Nawaf Alharthi, Raghad Mutir Alzahrani, Abdullah Nasir Alolyani, Salem Ahmed Salem Alshehri, Khalid Ali Alghamdi, Shahad Mansour Alharthi, Ali Hendi Al Ghamdi
DOI: http://dx.doi.org/10.52533/JOHS.2026.60304
Keywords: medical education, ophthalmology, career choice, Saudi Arabia, cross-sectional study
Background: Choosing a medical specialty is a critical milestone in medical education. Ophthalmology is a highly specialized field that combines microsurgical precision with the opportunity to significantly improve patients' quality of life. In Saudi Arabia, increasing demand for eye care services under Vision 2030 and the rising burden of diabetes-related eye disease highlight the need for a sustainable ophthalmology workforce. However, factors influencing medical students' interest in ophthalmology remain underexplored. This study aimed to identify motivators and barriers affecting Saudi medical students’ choice of ophthalmology as a future specialty.
Methods: A cross-sectional study was conducted among medical students at Albaha University in Saudi Arabia, during the 2024-2025 academic year. Data was collected using a self-administered, web-based questionnaire. The survey assessed demographic characteristics, academic level, specialty preferences, timing of specialty decision, exposure to ophthalmology, and factors influencing career choice. A total of 299 students from the second year through the internship year participated. Logistic regression analysis was performed to identify predictors of interest in ophthalmology.
Results: Among the 299 participants, 57.2% expressed interest in pursuing ophthalmology. Key motivating factors included personal interest, perceived lifestyle flexibility, and the opportunity to restore or improve vision. Major barriers included perceived residency competitiveness and the technical demands of the specialty. Early exposure to ophthalmology, particularly through clinical rotations and community service activities, was significantly associated with increased interest. Logistic regression analysis demonstrated that academic level, timing of specialty decision, and exposure to ophthalmology were significant predictors of interest in the field.
Conclusions: Early and sustained exposure to ophthalmology during medical training is strongly associated with increased student interest in the specialty. Addressing barriers such as perceived competitiveness and misconceptions about the field may enhance recruitment into ophthalmology. Curriculum-based interventions, structured mentorship, and expanded clinical exposure may support informed specialty decision-making and contribute to workforce sustainability in Saudi Arabia.
Introduction
As medical students progress through their education, they face a pivotal moment that rivals the significance of their initial decision to study medicine—choosing a specialty (1). This choice shapes their professional identity and fundamentally determines the rhythm of their future lives (2). Within the diverse landscape of medical specialties, ophthalmology is a distinct field that combines microsurgical precision with the profound responsibility of preserving and restoring one of humanity's most precious senses—vision (3).
The journey toward specialization in Saudi Arabian medical schools presents unique difficulties and opportunities. Medical students navigate through a complex web of influences, ranging from cultural expectations and family considerations to professional aspirations and personal interests (4, 5). Nevertheless, the path to ophthalmology often remains less traveled, not necessarily due to a lack of interest but potentially because of limited exposure during formative years in medical education.
The ophthalmological landscape of Saudi Arabia is especially intriguing. The demand for eye care specialists has considerably grown with the Kingdom continuing its rapid healthcare transformation under Vision 2030 (6). This growth coincides with rising rates of diabetes-related eye complications and an aging population, creating a compelling requirement for well-trained ophthalmologists (7). However, the factors that draw medical students toward or away from this specialty remain largely unexplored in Saudi Arabia.
Current medical education curricula often allocate minimal time to ophthalmology compared to broader specialties, such as internal medicine or surgery. This limited exposure creates a paradox. How can students make informed decisions regarding pursuing ophthalmology when their understanding of the field is likely incomplete? This challenge is compounded by the ophthalmic practice’s unique aspects, which combine outpatient care, intricate surgical procedures, and the opportunity to witness immediate improvements in patients' quality of life (8, 9).
The decision to pursue ophthalmology extends beyond a mere career choice; it reflects a commitment to mastering a highly specialized field that demands exceptional precision, continuous adaptation of the relevant technology, and a deep understanding of systemic diseases and their ocular manifestations (10). However, misconceptions regarding specialties may influence students' decisions before they have the opportunity to completely explore their scope and potential.
Despite existing studies on the factors influencing medical students’ specialty choices in Saudi Arabia, a notable lack of research exists that specifically focuses on ophthalmology. Thus, we aimed to identify the characteristics of ophthalmology that appeal to medical students and influence their decision-making processes by conducting a cross-sectional descriptive study among medical students. The insights gained from this investigation will enhance our understanding of what draws students to ophthalmology and will help shape how we introduce and teach this specialty to future generations of medical professionals in Saudi Arabia.
Methodology
Study Design, Setting
An observational cross-sectional study was performed on medical students at our center during the 2024–2025 academic year. This study involved 2nd-year students throughout their internship years to evaluate their perspectives on ophthalmology as a career choice.
Inclusion and Exclusion Criteria
All undergraduate medical students enrolled at our center from the second academic year through the internship year during the 2024–2025 academic year were eligible for inclusion in the study. Students were required to be actively registered and willing to provide informed consent to participate in the survey. First-year students were excluded, as they had not yet been sufficiently exposed to the medical curriculum or clinical specialties. Students from other institutions, postgraduate trainees, and incomplete questionnaire responses were also excluded from the final analysis.
Sampling Procedures
The necessary sample size for this study was 346 students, determined using the cross-sectional study design formula for a finite population, given that our center had approximately 1,000 enrolled students. The formula used was n = [1 + {([Z²P (1 − P)]/d² − 1)/Pop}]. We set p = 50%, which yielded an initial sample size of 275 using the equation without previous data regarding the proportion of students interested in ophthalmology as a future career, and targeted an error margin of no greater than 5% at a 95% confidence interval. We increased the sample size by 25% to account for the potential non-response rates commonly linked to web-based surveys, leading to a final target of 346 undergraduate students.
This study used stratified random sampling, with each academic year representing a distinct stratum. Students were selected from the 2nd year through the internship year, with the sample size equally distributed across these years owing to the relatively uniform number of students in each academic cohort. This ensured representative sampling.
Data Collection and Instrumentation
Data were collected using a web-based, self-administered questionnaire designed to capture comprehensive information on the attitudes of students toward ophthalmology. The questionnaire used in this study was adapted from previously validated surveys conducted in an analogous research effort that investigated the factors influencing medical students’ choice of ophthalmology as a career (11, 12). The questionnaire was divided into three main sections. The first section gathered demographic information, including sex, age, current academic year, marital status, academic performance (grade point average [GPA]), and the top three specialty preferences. The second section included various factors influencing career choices, such as personal interest in ophthalmology, expected income potential, lifestyle considerations, private practice opportunities, technical aspects of ophthalmic procedures, clinical diagnostic requirements, routine work preferences, patient satisfaction metrics, and disease prognosis considerations. The final section evaluated the students’ exposure to ophthalmology through their experiences with ophthalmic procedures, participation in relevant conferences, research involvement, and community service activities.
The questionnaire was validated via expert reviews conducted by board-certified ophthalmologists and medical educators. A pilot study was performed with 20 students to test clarity and reliability, and minor revisions were made based on the feedback received.
Statistical Analysis
The collected data underwent two analysis levels. Initially, we conducted descriptive statistics and calculated the frequencies, percentages, and standard errors of the sample variables to present a comprehensive overview of the dataset. Subsequently, logistic regression analysis was used to identify the significant predictors of choosing ophthalmology as a future specialization. Crude odds ratios (ORs) and 95% confidence intervals (CIs) were calculated. All analyses were performed using IBM SPSS Statistics for Windows (version 24.0; IBM, Armonk, NY, USA), with statistical significance set at p < 0.05 for all two-sided tests.
Ethical Considerations
This study was conducted in accordance with the principles of the Declaration of Helsinki. Ethical approval was obtained from the Institutional Review Board (IRB) of the Faculty of Medicine, Al-Baha University, Saudi Arabia (Approval No.: IRB/SUR/BU-FM/2024/125; Approval Date: 27/11/2024). Informed consent was obtained electronically from all participants prior to enrollment. Participants were informed of the study objectives and their right to withdraw at any time without consequence. All data was collected anonymously and handled confidentially in accordance with institutional research ethics guidelines.
Results
General Characteristics of Study Participants
A total of 299 medical students participated in the study, with 40.1% women and 59.9% men (Table 1). Among the participants, 57.2% expressed a desire to choose ophthalmology as their future specialty. Sex did not significantly influence this preference (p = 0.27). The age groups demonstrated a significant difference, with younger students (<21 years) being more likely to choose ophthalmology (66.2%, p = 0.03). Additionally, academic level played a significant role (p = 0.003), with 3rd-year students showing the highest interest (76.3%), whereas interest declined among the 6th-year students (38.6%). Marital status and GPA did not significantly influence the choice of ophthalmology. The timing of decision-making for specialty preference was significant (p = 0.003), with students deciding before medical school (70.9%) being more likely to prefer ophthalmology than those deciding during the clinical years (45.4%).
|
Table 1: General characteristics of the study participants and their desire to choose ophthalmology as a future career |
||||
|
Characteristic |
All participants N (%) |
Desire to choose Ophthalmology as a future career N (%) |
p-value |
|
|
Sex |
Women |
120 (40.1%) |
64 (53.3%) |
0.27 |
|
Men |
179 (59.9%) |
107 (59.8%) |
||
|
Age groups |
<21 years |
68 (22.7%) |
45 (66.2%) |
0.03 |
|
21–22 years |
102 (34.1%) |
63 (61.8%) |
||
|
≥23 years |
129 (43.1%) |
63 (48.8%) |
||
|
Marital status |
Married |
8 (2.7%) |
5 (62.5%) |
0.75 |
|
Single |
291 (97.3%) |
166 (57.0%) |
||
|
Academic level |
2nd year |
47 (15.7%) |
31 (66.0%) |
0.003 |
|
3rd year |
38 (12.7%) |
29 (76.3%) |
||
|
4th year |
65 (21.7%) |
42 (64.6%) |
||
|
5th year |
47 (15.7%) |
25 (53.2%) |
||
|
6th year |
57 (19.1%) |
22 (38.6%) |
||
|
Internship |
45 (15.1%) |
22 (48.9%) |
||
|
CGPA |
<3 |
90 (30.1%) |
53 (58.9%) |
0.56 |
|
3–3.5 |
86 (28.8%) |
37 (43.02%) |
||
|
3.5–4 |
123 (41.1%) |
45 (36.6%) |
||
|
When Did You Make Your Specialty Preference? |
Before medical school |
55 (18.4%) |
39 (70.9%) |
0.003 |
|
During basic science |
50 (16.7%) |
33 (66.0%) |
||
|
During clinical years |
130 (43.5%) |
59 (45.4%) |
||
|
Others |
64 (21.4%) |
40 (62.5%) |
||
|
All medical students |
299 (100%) |
171 (57.2%) |
||
Specialty Preferences among Medical Students
Figure 1 provides a detailed visualization of the ranking of the chosen specialty preferences among the medical students for their first, second, and third choices. Internal medicine was the most frequently chosen specialty across all ranks, especially as the first choice, where 11.7% of participants selected it. Ophthalmology was closely followed as the second most preferred first-choice specialty at 9.7%, and general surgery, including its subspecialties, ranked third at 8.4%. Regarding second-choice preferences, internal medicine retained its leading position (16.4%), followed by ophthalmology (10.4%) and dermatology (8.0%). This indicated continued interest in these specialties, even as secondary options. For the third-choice preferences, a notable shift occurred, with “undecided” emerging as the most common response (14.7%), suggesting uncertainty or openness among students regarding their future career paths. Family and internal medicine were the second-most popular third-choice preferences, each accounting for 8.7% of the responses. Additionally, specialties such as ophthalmology (6.7%), orthopedics (6.0%), and pediatrics (6.0%) were commonly chosen as third preferences, indicating their appeal as fallback options for several students.
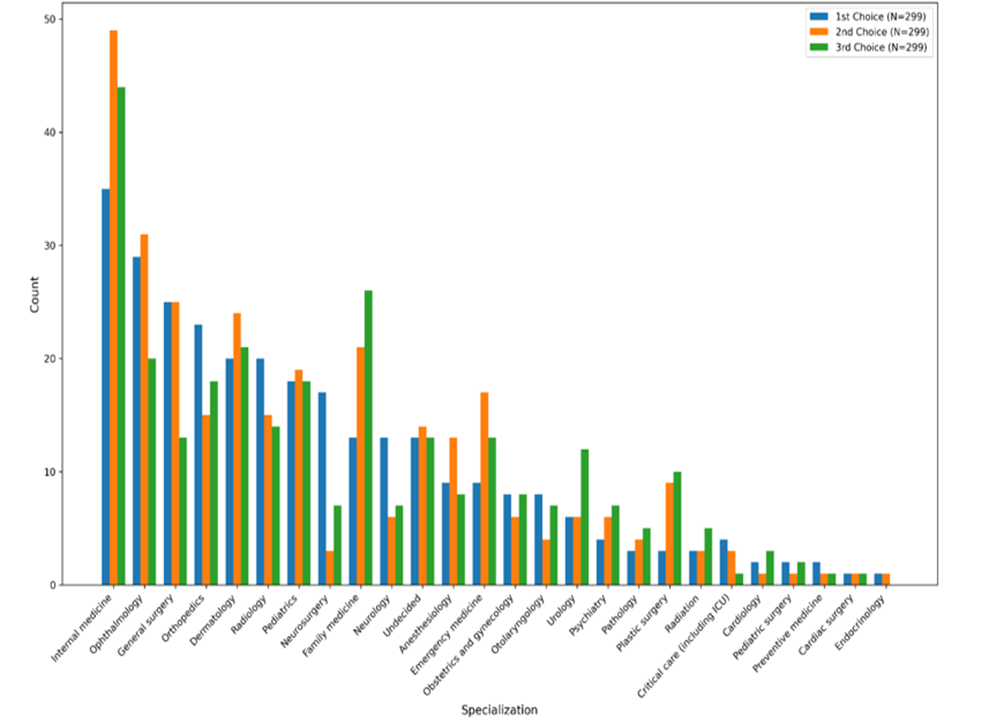
Figure 1: Ranking of the chosen specialty choices among medical students
Factors Influencing Career Choice in Ophthalmology
Table 2 lists the factors that influenced students’ decisions to pursue ophthalmology. Personal interest was the most influential factor, with 66.7% agreeing and 22.2% strongly agreeing. Furthermore, high income and lifestyle flexibility were significant motivators, with 59.1% and 49.1% agreeing, respectively. Other important factors included the opportunity to perform the procedures (57.9% agreed) and the perception of good patient prognosis (53.2% agreed). Contrastingly, factors such as the challenge of obtaining residency (36.8% agreed) and the degree of stress (39.2% agreed) were less influential.
|
Table 2: Factors influencing career choice in ophthalmology |
|||||
|
Factor |
Strongly Agree (N, %) |
Agree (N, %) |
Neutral (N, %) |
Disagree (N, %) |
Strongly Disagree (N, %) |
|
Personal interest |
38 (22.2%) |
114 (66.7%) |
12 (7.0%) |
1 (0.6%) |
6 (3.5%) |
|
High income |
44 (25.7%) |
101 (59.1%) |
13 (7.6%) |
9 (5.3%) |
4 (2.3%) |
|
Your GPA |
24 (14.0%) |
88 (51.5%) |
26 (15.2%) |
24 (14.0%) |
9 (5.3%) |
|
The appeal of being an ophthalmologist |
30 (17.5%) |
94 (55.0%) |
22 (12.9%) |
18 (10.5%) |
7 (4.1%) |
|
The desire for little contact with emergency situations |
37 (21.6%) |
83 (48.5%) |
19 (11.1%) |
27 (15.8%) |
5 (2.9%) |
|
The degree of stress |
48 (28.1%) |
67 (39.2%) |
23 (13.5%) |
26 (15.2%) |
7 (4.1%) |
|
Lifestyle/flexible work schedule |
59 (34.5%) |
84 (49.1%) |
13 (7.6%) |
8 (4.7%) |
7 (4.1%) |
|
The opportunity to perform procedures |
30 (17.5%) |
99 (57.9%) |
15 (8.8%) |
20 (11.7%) |
7 (4.1%) |
|
Relies on clinical diagnostic skills |
32 (18.7%) |
101 (59.1%) |
19 (11.1%) |
14 (8.2%) |
5 (2.9%) |
|
Routine work/small range of medical problems |
40 (23.4%) |
86 (50.3%) |
15 (8.8%) |
25 (14.6%) |
5 (2.9%) |
|
The difficulty of getting into ophthalmology residency |
36 (21.1%) |
63 (36.8%) |
24 (14.0%) |
30 (17.5%) |
18 (10.5%) |
|
The likelihood that an ophthalmologist can influence patients’ lives |
41 (24.0%) |
83 (48.5%) |
17 (9.9%) |
22 (12.9%) |
8 (4.7%) |
|
Good patient prognosis |
43 (25.1%) |
91 (53.2%) |
20 (11.7%) |
11 (6.4%) |
6 (3.5%) |
|
Personal satisfaction from helping people to see better |
56 (32.7%) |
89 (52.0%) |
11 (6.4%) |
11 (6.4%) |
4 (2.3%) |
|
The geographic location of the training center |
23 (13.5%) |
75 (43.9%) |
34 (19.9%) |
17 (9.9%) |
22 (12.9%) |
|
Duration of the training |
25 (14.6%) |
93 (54.4%) |
30 (17.5%) |
17 (9.9%) |
6 (3.5%) |
|
Research opportunities |
24 (14.0%) |
84 (49.1%) |
35 (20.5%) |
19 (11.1%) |
9 (5.3%) |
|
Variety of the cases and population character |
23 (13.5%) |
90 (52.6%) |
32 (18.7%) |
18 (10.5%) |
8 (4.7%) |
|
Having a role model |
19 (11.1%) |
84 (49.1%) |
33 (19.3%) |
23 (13.5%) |
12 (7.0%) |
|
Number of On-calls |
27 (15.8%) |
78 (45.6%) |
33 (19.3%) |
21 (12.3%) |
12 (7.0%) |
|
The need for the specialty in the market |
26 (15.2%) |
84 (49.1%) |
35 (20.5%) |
20 (11.7%) |
6 (3.5%) |
|
The need for ICU admission in ophthalmology is minimal |
29 (17.0%) |
76 (44.4%) |
32 (18.7%) |
27 (15.8%) |
7 (4.1%) |
|
The risk to a patient’s life in ophthalmology is low |
29 (17.0%) |
78 (45.6%) |
29 (17.0%) |
25 (14.6%) |
10 (5.8%) |
|
Most ophthalmology cases managed on outpatient basis |
36 (21.1%) |
82 (48.0%) |
28 (16.4%) |
24 (14.0%) |
1 (0.6%) |
|
Patient outcomes are typically favorable |
35 (20.5%) |
94 (55.0%) |
20 (11.7%) |
19 (11.1%) |
3 (1.8%) |
|
Wide range of sub-specialties |
26 (15.2%) |
92 (53.8%) |
31 (18.1%) |
16 (9.4%) |
6 (3.5%) |
|
Post-graduation training length is manageable |
27 (15.8%) |
93 (54.4%) |
33 (19.3%) |
12 (7.0%) |
6 (3.5%) |
|
Feasibility of private clinic |
49 (28.7%) |
81 (47.4%) |
20 (11.7%) |
15 (8.8%) |
6 (3.5%) |
|
Use of innovative technologies |
42 (24.6%) |
90 (52.6%) |
16 (9.4%) |
20 (11.7%) |
3 (1.8%) |
|
Interface with other areas of medicine |
22 (12.9%) |
87 (50.9%) |
35 (20.5%) |
23 (13.5%) |
4 (2.3%) |
Exposure to Ophthalmology
Table 3 summarizes the participants’ exposure to ophthalmology and related activities. The majority (39.8%) were exposed to ophthalmology during the clinical and basic years, whereas 33.3% reported no exposure. More than half (61.4%) had never participated in an ophthalmic procedure, and 56.1% did not. Regarding conferences, 40.4% expressed interest in attending, whereas only 19.3% attended them. Similarly, 26.3% indicated an interest in ophthalmology research, with 29.8% participating. Community service activities associated with ophthalmology were limited, with 42.7% of participants reporting no involvement.
|
Table 3: Participants’ exposure to ophthalmology and related activities |
||
|
Question |
Response |
Count (%) N = 171 |
|
Have you ever been exposed to ophthalmology? |
Neither |
57 (33.3%) |
|
Yes, in basic years |
46 (26.9%) |
|
|
Yes, in clinical and basic years |
68 (39.8%) |
|
|
Have you ever been exposed to an ophthalmic procedure? |
No |
105 (61.4%) |
|
Yes |
66 (38.6%) |
|
|
Have you ever observed an ophthalmic procedure? |
No |
96 (56.1%) |
|
Yes |
75 (43.9%) |
|
|
Have you ever attended a conference in ophthalmology? |
I would like to |
69 (40.4%) |
|
No |
50 (29.2%) |
|
|
Not my priority |
19 (11.1%) |
|
|
Yes |
33 (19.3%) |
|
|
Have you ever participated in ophthalmology research? |
I would like to |
45 (26.3%) |
|
No |
65 (38.0%) |
|
|
Not my priority |
10 (5.8%) |
|
|
Yes |
51 (29.8%) |
|
|
Have you ever participated in any community service activity related to ophthalmology? |
I would like to |
41 (24.0%) |
|
No |
73 (42.7%) |
|
|
Not my priority |
7 (4.1%) |
|
|
Yes |
50 (29.2%) |
|
Independent Predictors for Choosing Ophthalmology
Logistic regression analysis identified the main predictors of ophthalmology as a future specialty (Table 4). The academic level was a significant predictor, with 6th-year students being less likely to choose ophthalmology compared to 2nd-year students (OR = 0.13, 95% CI = 0.03–0.56, p = 0.01). Similarly, interns were less likely to choose ophthalmology (OR = 0.18, 95% CI = 0.04–0.84, p = 0.03). Students deciding their specialty preference during clinical years were less likely to choose ophthalmology compared to those deciding before medical school (OR = 0.45, 95% CI = 0.21–0.97, p = 0.04). In the multivariate analysis, sex, marital status, GPA, and age were not significant predictors.
|
Table 4: Logistic regression analysis of independent predictors for choosing ophthalmology as a future specialty |
||
|
Variables |
Multivariate Regression OR (95% CI) |
p-Value |
|
Sex |
||
|
Female (reference) |
1 (r) |
0.24 |
|
Male |
1.3 (0.8–2.2) |
|
|
Marital Status |
||
|
Single (reference) |
1 (r) |
0.58 |
|
Married |
1.5 (0.3–7.1) |
|
|
Age |
||
|
<21 years (reference) |
1 (r) |
0.39 |
|
21–22 years |
1.6 (0.57–4.32) |
0.37 |
|
≥23 years |
2.453 (0.67–8.9) |
0.17 |
|
Level of Study |
||
|
2nd year (reference) |
1 (r) |
0.03* |
|
3rd year |
1.3 (0.47–3.6) |
0.59 |
|
4th year |
0.6 (0.19–1.84) |
0.36 |
|
5th year |
0.3 (0.08– 1.14) |
0.07 |
|
6th year |
0.13 (0.03–0.56) |
0.01* |
|
Internship |
0.18 (0.04–0.84) |
0.03* |
|
GPA |
||
|
<3 |
1 (r) |
0.89 |
|
3–3.5 |
1.2 (0.61–2.2) |
0.64 |
|
3.5–4 |
1.09 (0.59–1.9) |
0.77 |
|
When Did You Make Your Specialty Preference? |
||
|
Before medical school |
1 (r) |
0.21 |
|
During basic science |
0.68 (0.28–1.62) |
0.38 |
|
During clinical years |
0.45 (0.21–0.97) |
0.04* |
|
Others |
0.7 (0.31–1.57) |
0.38 |
Discussion
Our study investigated factors influencing medical students’ decisions to pursue ophthalmology as a future specialty in the medical education system of Saudi Arabia. This study provides valuable insights into how students navigate the difficulties and opportunities linked to this prestigious field.
Our findings indicated that 57.2% of participants expressed an interest in ophthalmology as a future career, underscoring the notable interest in this specialty. This is in line with the studies by Al-Barry et al. (2021) and Madani et al. (2018), who identified ophthalmology as a less popular and competitive specialty (11, 12). However, the proportion of students who ranked ophthalmology as their first choice in this study (6.1%) was higher than the 5.6% reported by Madani et al. This reflects a recent, slow-growing interest in ophthalmology. Similar trends have also been reported in other studies among medical students, suggesting that interest in ophthalmology is gradually increasing despite the competitiveness of the specialty.
Personal interest emerged as the most significant factor affecting specialty choice, consistent with Al-Barry et al.’s findings emphasizing the role of intrinsic motivation in career decision-making. Furthermore, academic level and timing of specialty preference were significant predictors for choosing ophthalmology. This study showed that age and academic level considerably affected the desire to pursue ophthalmology. Younger students (<21 years) and those at earlier academic levels, especially 2nd- and 3rd-year students, were more likely to prefer ophthalmology. Senior students (6th-year students and interns) were less likely to choose ophthalmology, likely owing to greater exposure to alternative specialties or a shift in priorities. This may reflect optimism and broader exploration of career possibilities among junior students as opposed to senior students, who may have developed preferences based on clinical rotations or other factors (13). These results are consistent with those of previous research suggesting that early exposure to a specialty positively influences career decisions (14). Additionally, students who made their specialty decisions before joining medical school were more inclined to pursue ophthalmology, underscoring the role of early career aspirations and the requirement for targeted outreach for pre- and junior medical students (19). Furthermore, exposure to ophthalmology during the clinical and basic years was reported by 39.8% of the participants, whereas 33.3% had no exposure. This underscores the importance of integrating ophthalmology rotations and related activities such as conferences, research, and community services into the medical curriculum. Students who participated in ophthalmology-related activities showed a higher interest in the specialty, consistent with studies by Madani et al. and Chen et al., which highlighted the influence of positive experiences and early engagement on career preferences (12, 15). This finding is also supported by international studies that highlight the importance of early clinical exposure and mentorship in influencing medical students’ specialty preferences.
Consistent with Al-Barry et al.’s study, personal satisfaction from improved vision and a good prognosis of ophthalmology cases were key motivators for students. Lifestyle considerations such as flexible work schedules and minimal emergency demands were also significant factors, echoing findings of Madani et al. and Savur et al (16). These lifestyle attributes make ophthalmology appealing, especially for students prioritizing work-life balance, a growing trend among medical graduates globally. Conversely, barriers such as difficulty of securing residency positions and perceived reliance on fine motor skills were deterrents for some students (17). These challenges align with results from studies by Savur et al. and others that identified the competitive nature of ophthalmology residency programs and misconceptions about the specialty as obstacles to recruitment (18).
Sex, marital status, and GPA did not demonstrate substantial associations with the choice of ophthalmology, in contrast to Madani et al.’s findings of a female preponderance among students interested in ophthalmology (12). This discrepancy may be attributed to differences in the study populations or shifts in sex dynamics over time.
The above results suggest that academic level, internship experience, and timing of specialty choice play critical roles in medical students’ decisions regarding ophthalmology. The finding that students and interns in later years are less likely to choose ophthalmology as a specialty highlights the importance of early, continuous exposure, especially given the growing global demand for ophthalmologists.
The high ranking of internal medicine as the first choice among medical students (11.7%) can be attributed to several factors. The field's breadth and scope, encompassing diverse patient populations and clinical settings, may appeal to students seeking a wide range of experiences and intellectual challenges. Additionally, diverse career paths within internal medicine, including general practice and various sub-specialties, provide flexibility and allow students to tailor their careers according to evolving interests. This versatility may be attractive for students exploring specific career goals in medicine. Furthermore, the perceived accessibility of internal-medicine residency positions, with more available spots than in competitive specialties, could affect student choices, possibly making it a more attainable goal for students in the context of the competitive residency application process. Notably, while factors like ease of acceptance and seat availability play a role, they do not completely explain internal medicine’s popularity. Several students are genuinely drawn to the intellectual challenges, patient interactions, and opportunities to provide comprehensive patient care in this field.
Thus, addressing barriers like residency competitiveness and misconceptions could help attract more students to ophthalmology. Integrating early ophthalmology rotations and offering hands-on experience, mentorship, and exposure to technological advancements may inspire interest among students. Furthermore, students from rural or underserved areas may have limited opportunities, as residency positions are often in larger cities (7,20). Thus, expanding training programs and promoting rural practices can help address workforce imbalances.
Strengths
This study possesses several strengths. First, it included students across multiple academic levels, from pre-clinical years to internship, allowing for a comprehensive assessment of how perspectives evolve throughout medical training. Second, the use of stratified random sampling enhanced the representativeness of the sample. Third, the questionnaire was adapted from previously validated instruments and underwent expert review and pilot testing, strengthening its methodological rigor. Furthermore, the use of multivariate logistic regression enabled identification of independent predictors while controlling potential confounders.
Limitations
This study had some limitations. First, its cross-sectional design precludes establishing causal relationships between factors and career preferences. Second, the study relied on self-reported data, which may have introduced recall or social desirability bias. Third, the sample was limited to medical students from selected institutions, which may have affected the generalizability of the findings to other regions or countries. Fourth, the study did not include postgraduate trainees whose career preferences may vary owing to additional exposure and experience. Lastly, the influences of faculty, mentors, and clinical rotations on specialty choices were not explicitly evaluated, warranting further investigation.
Recommendation
Based on the findings, several recommendations can be proposed. Early integration of structured ophthalmology exposure within the medical curriculum may help sustain students’ interest. Incorporating dedicated ophthalmology rotations, simulation-based procedural workshops, mentorship programs, and research opportunities may positively influence career decisions. Additionally, addressing misconceptions regarding residency competitiveness and technical demands through academic advising and career counseling could improve recruitment into the specialty. Expanding outreach initiatives targeting junior medical students and even pre-medical students may further support long-term workforce sustainability in ophthalmology within Saudi Arabia.
Conclusion
This study highlights factors influencing Saudi medical students’ choice of ophthalmology: personal interest, lifestyle flexibility, and improving vision were key motivators, while residency competitiveness and technical challenges were barriers. Early exposure and positive experiences (rotations, research, community service) increased interest in ophthalmology. The study results emphasize the implementation of targeted interventions, such as enhancing early exposure and correcting misconceptions, to attract students and ensure a sustainable ophthalmology workforce in Saudi Arabia.
Disclosure
Funding
This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflict of interest
There is no conflict of interest.
Ethical consideration
This study was conducted in accordance with the principles of the Declaration of Helsinki. Ethical approval was obtained from the Institutional Review Board (IRB) of the Faculty of Medicine, Al-Baha University, Saudi Arabia (Approval No.: IRB/SUR/BU-FM/2024/125; Approval Date: 27/11/2024).
Author contribution
All authors contributed equally to the conceptualization, data collection, data analysis and writing of the paper.
Data availability
All data is available within the manuscript.